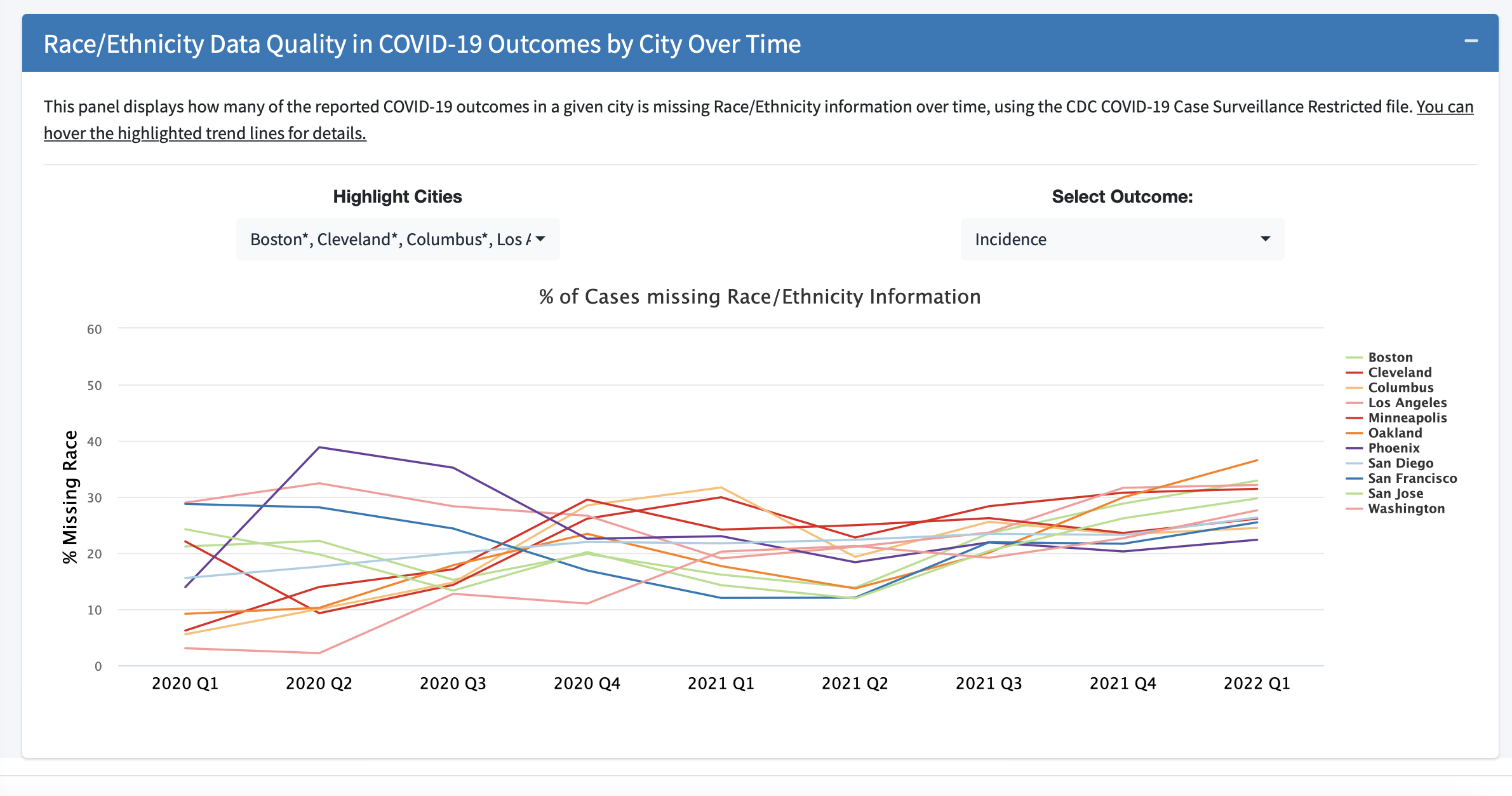
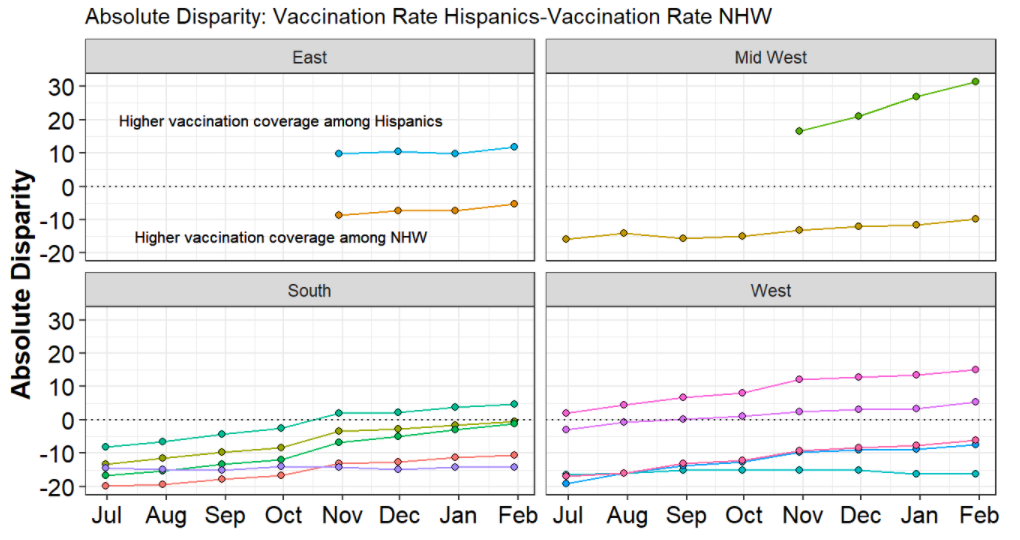
CITIES, INEQUITIES AND COVID-19: THE CREATION OF A DASHBOARD
Population health challenges in urban areas have been heightened by the ongoing COVID-19 pandemic. The United States population largely lives in cities. While the pandemic affected the entire country, cities were initially the hardest hit. Cities are especially vulnerable to pandemics, as they have a greater population density, generally have larger inequality gaps, and see more travelers from across the country and world. However, at the same time, cities concentrate resources that can help mitigate public health emergencies.